California COVID Peak Expected April 15, New Cases Still Rising
The San Francisco Bay Area has seen a slight but steady, increase in the number of COVID-19 patients over the last week. According the numbers reported by John Hopkins Coronavirus Resource Center, on April 2nd there were 2,495 total confirmed COVID-19 cases across all 6 Bay Area counties, 7 days later on April 8th, the total cases in the Bay Area had grown to 4,206 confirmed cases.
That number is expected to continue to grow this week, but not at a rate that threatens to overwhelm our hospitals and ICU’s. According to the Institute for Health Metrics and Evaluation (IHME), California currently has enough hospital beds to accommodate its predicted growth in new COVID cases. So far, the Bay Area and California as a whole has ‘flattened the curve’ of new infections. Next week will be the real challenge, when the rate of infections is predicted to peak in the State.
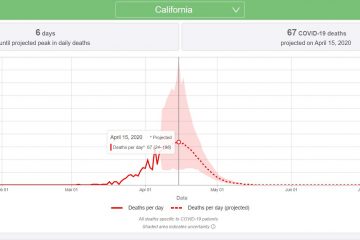
COVID Peak in California is predicted to begin and end next week April 13th-17th:

The Institute for Health Metrics and Evaluation (IHME) predicts California will have it’s COVID death ‘peak’next week. Daily deaths should begin to go down around 4/16.
COVID cases and deaths across the state of California are predicted to grow for at least another week, the peak of COVID related deaths in the state is expected on April 15th, bus based on comparing predicted COVID cases to the number of available hospital and ICU beds across the state IHME estimates California will not run out of hospital beds.
In short, the worse is yet to come, but California can consider itself very lucky that our leaders in the public and private sector instituted the shelter in place order early (March 19th). This decision most likely saved thousands of lives by drastically lowering the rate of new infections.
The largest amount of confirmed cases in California remains in the Los Angeles area, with 7,573 confirmed cases as of April 9th, 2020. New York City remains the hardest hit in the nation with 81,803 confirmed but their rate of infection in NYC is expected to go down starting today, April 9th.

John Hopkins University Coronavirus Resource Center Map
Total Confirmed COVID cases in United States 4/9/2020: 432,554
For confirmed COVID cases around the country and the world, reference The John Hopkins University COVID Map here.
Bay Area Status Report
To see how things are going on the ground in the Bay Area, and to put these numbers into perspective we followed up with Dr. Nathan Teismann of the UCSF Emergency Medicine Department. Dr. Teismann was working in the UCSF ER this morning, April 9, and was nice enough to answer our questions. When asked if he had seen an increase in COVID patients in his ER this week, Dr. Teismann wrote:
“Slightly but not significantly. In the UCSF ER, our overall patient volumes continue to be fairly low, roughly a third to a half of normal, which has been consistent over the past few weeks. We have around 20 patients admitted to the hospital right now with confirmed cases, and about half of those are in the ICU. We’re obviously still prepared for a significant uptick in patients who will need care over the next few weeks, but overall we’re very grateful that things here remain pretty manageable.”
Dr. Teismann has contacts in other ER’s in San Francisco as well as on the Peninsula and in the East Bay, we asked him how his colleagues at other hospitals are doing. Dr. Teismann replied: “The colleagues I’ve spoken to in other local ER’s report similar situations – basically that they are seeing and testing a slightly increasing number of patients for Covid, but that overall things are still under control. Obviously it’s too early to say this with any certainty, but there is real hope that we’ll be able to weather the storm, both in SF and across the Bay Area.”
BAS: Do you all have enough PPE equipment?
Dr. Teismann: “We’re still being very conservative and re-using PPE as much as we can, but overall we’re doing OK. Actually a group of our engineers, MD’s and some of our students team are using 3D printers to mass-produce medical face shields for our hospitals, which is fantastic.”
BAS: Any updates on COVID testing technology or techniques?
Dr. Teismann: “The big thing at this point is that we’re looking to develop serologic testing for an immune response to COVID. In other words, testing for antibodies that would indicate that someone has recovered and presumably is protected from becoming infected again. This also has therapeutic potential, meaning that these protective antibodies could be given as an infusion from patients who have recovered to patients who are critically ill.”
In conclusion, sheltering in place is having a dramatic effect by slowing the spread of the virus. Unfortunately not everyone has a place to shelter, especially those living on our streets. The brave people doing necessary jobs during this time are also still at great risk. Our grocery store workers, our firemen, our plumbers, our fry cooks, our truckers, and our doctors and nurses. Until we have widespread, comprehensive testing available to everyone, the rest of us will not be able to go to work or attend concerts, or take an airplane. For the foreseeable future, we must stay put.
Keep sheltering in place, we are doing incredibly well with social distancing, so keep it up!